Aptamil and Neocate Syneo Range
There’s a growing body of research investigating gut microbiota - the community of bacteria living in the gut - and immune responses and outcomes. As such, we’re getting a better understanding of the benefits of modulating gut microbiota when managing Cow’s Milk Allergy (CMA), sometimes known as Cow’s Milk Protein Allergy (CMPA), in formula fed infants.
The potential role of synbiotics in the management of CMA is becoming increasingly clear. In this article, we discuss what synbiotics are, the connection between the gut microbiota and the immune system, and how this science may shape the future of cow’s milk allergy management.
What are synbiotics?
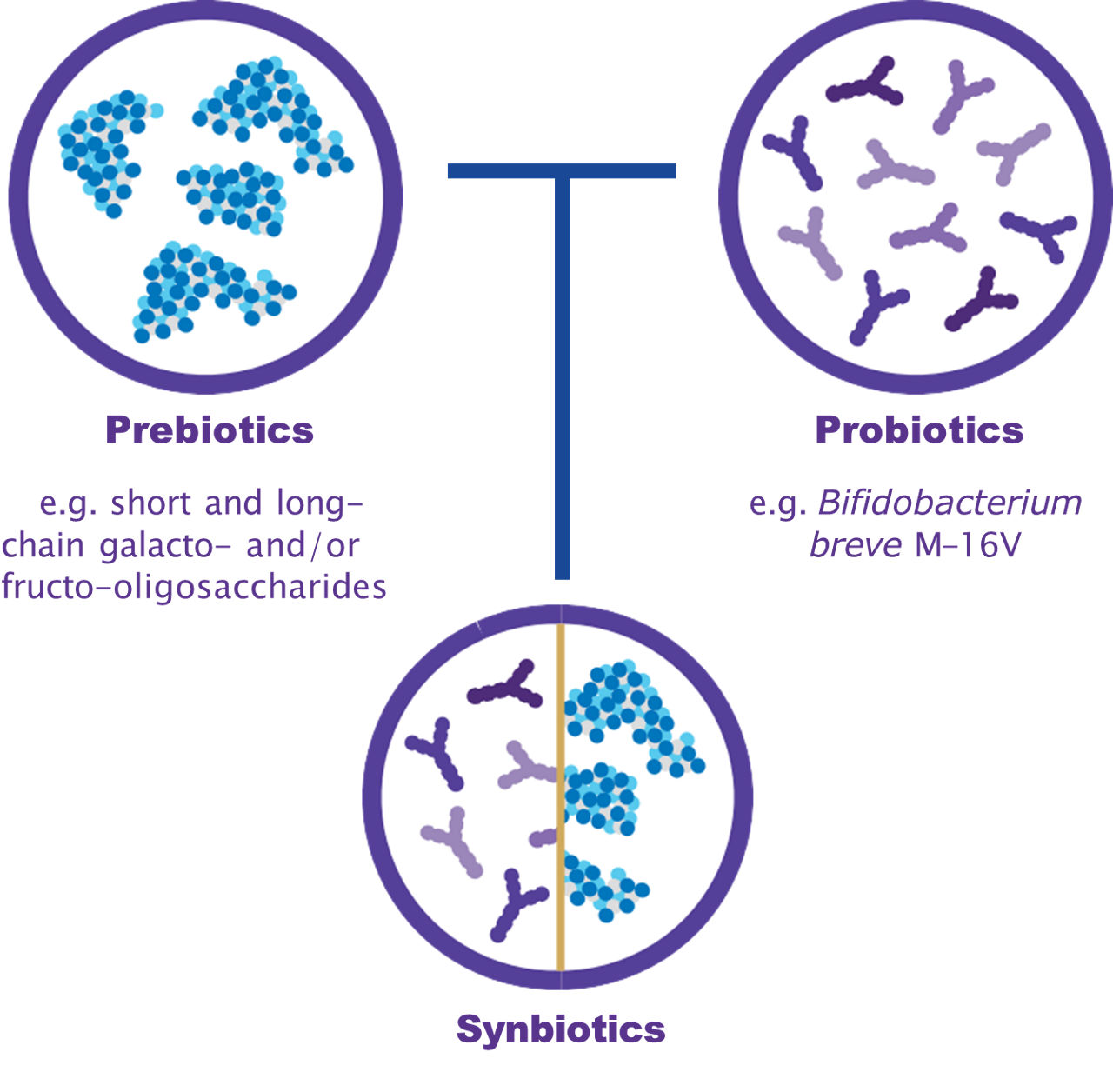
Synbiotics combine prebiotics and probiotics¹⁻². Although the two are sometimes confused, they have distinct functions:
- Prebiotics are non‑digestible food ingredients that stimulate the growth or activity of beneficial gut bacteria³.
- Probiotics are beneficial bacteria that can help rebalance gut microbiota when consumed in adequate amounts⁴⁻⁵.
The goal of combining prebiotics and probiotics is to produce a synergistic effect, offering greater benefits together than either component alone⁶.
Gut microbiota and immune system development
With 70–80% of immune cells located in the gut⁷, the gut microbiota and immune system are closely interconnected.
From the moment we’re born, gut microbiota play a very important role when it comes to immune system development and its responses8-9. At birth, the gut is essentially sterile and not yet populated with the diverse microbiota required for a healthy microbiome⁶. Colonisation begins immediately after birth, diversifies with the introduction of solid foods, and typically matures by around age three⁸⁻⁹.
The immune system is also immature at birth and continues to develop as it learns to distinguish harmful threats from beneficial exposures. Working together, the gut microbiota and immune system help:
- Defend against harmful pathogens
- Maintain immune tolerance to antigens¹⁰
- Strengthen overall immune defences¹¹
In infants and young children, maintaining a healthy balance between gut microbiota and immune function is particularly important, as it influences lifelong health trajectories¹².
What causes gut dysbiosis?
Gut dysbiosis refers to an imbalance in the gut microbiota¹³ and is associated with a range of conditions, including inflammatory bowel disease, obesity, type 1 diabetes, and allergic disorders¹⁴⁻¹⁵.
Many factors can contribute to dysbiosis, such as diet, antibiotic use, complementary feeding, and physical or psychological stress¹⁶. Early life is a particularly vulnerable period, with key risk factors including¹⁷⁻¹⁸:
- Premature birth
- Caesarean delivery
- Antibiotic exposure
Microbiome and allergies: the impact of gut microbiota dysbiosis on health and the development of Cow’s Milk Allergy
Healthy breastfed infants typically have higher levels of Bifidobacteria, a beneficial probiotic passed on during birth and through breast milk¹⁹⁻²⁰. Breast milk also contains non‑digestible oligosaccharides—complex carbohydrates readily consumed by Bifidobacteria²¹.
Infants with cow’s milk allergy often show gut dysbiosis, characterised by significantly reduced Bifidobacteria and increased levels of more adult‑like bacteria²²⁻²³.
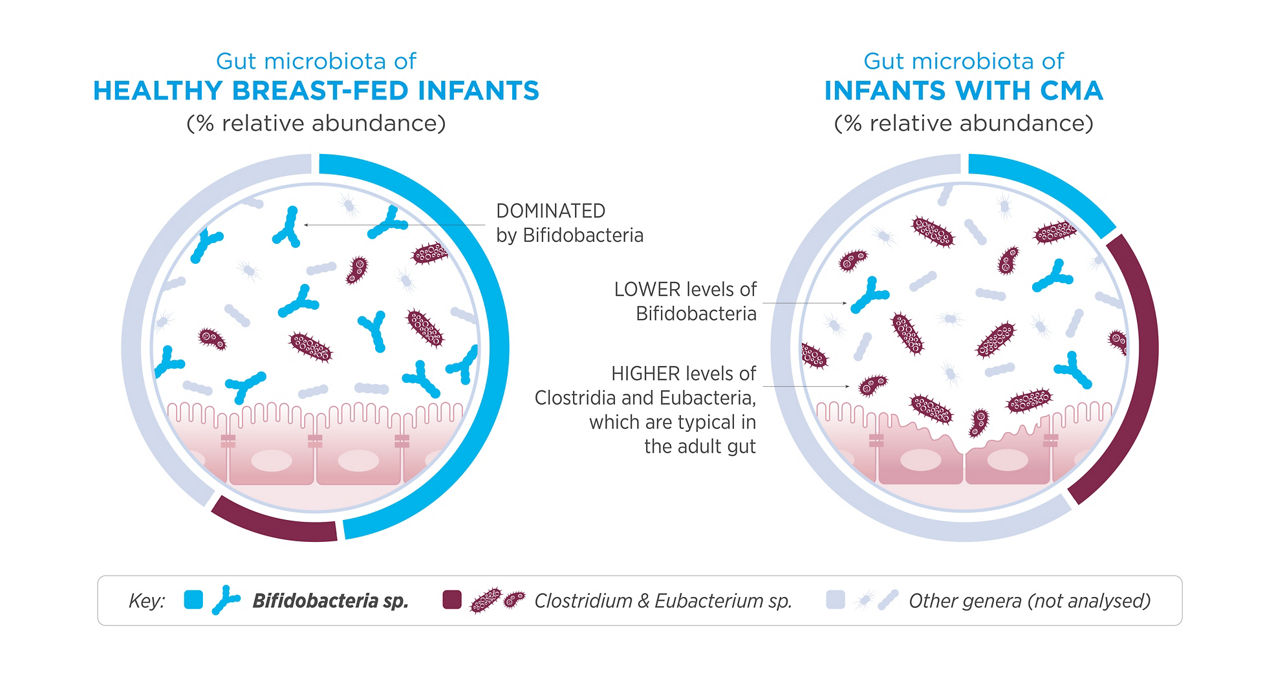
This imbalance can trigger abnormal immune responses, which in turn can potentially contribute to the development of food allergies, including Cow’s Milk Allergy¹⁵,²².
Synbiotics and the management of Cow’s Milk Allergy
Cow’s Milk Allergy occurs when the immune system reacts abnormally to cow’s milk protein26. It typically develops within the first few months of life and affects 2–3% of infants under one year27.
Some studies suggest synbiotics may help regulate the gut microbiota and immune responses—both directly and indirectly24. They may also help manage and reduce the severity of CMA symptoms25,29.
Future of Cow’s Milk Allergy management
Current management primarily involves removing cow’s milk protein from the infant’s diet. For symptomatic breastfed infants, mothers are usually advised to follow a dairy‑free diet to avoid transferring cow’s milk protein through breast milk27-28. For formula fed or mixed fed infants, hypoallergenic formula are recommended. 1,26,27
While this approach is effective at reducing symptoms, synbiotics may play a valuable role in future management strategies. By helping to rebalance the gut microbiota, synbiotics may address the underlying dysbiosis that contributes to abnormal immune responses and allergy development1.
Aptamil and Neocate SYNEO Range
The SYNEO range is the only hypoallergenic formula range for the dietary management of Cow’s Milk Allergy that contains synbiotics—a unique blend of prebiotics and probiotics.30*

With SYNEO, the benefits stack up.
- Contains more of the gut microbiota modulating factors found in breastmilk than any other hypoallergenic formula30†
- Rebalances the gut microbiota23, 31-35 to support immune development and long‑term health36-41
- Clinically shown to deliver both short‑ and long‑term benefits25,29,34-36‡
Discover the only hypoallergenic formula range with synbiotics.*†
- Fox, et al. World Allergy Organ J. 2019;12(5):100034.
- Swanson, et al. Nat Rev Gastroenterol Hepatol. 2020;17(11):687-701
- Gibson, et al. Nat Rev Gastroenterol Hepatol. 2017;14(8):491-502.
- Hill, et al. Nature Reviews Gastroenterology & Hepatology. 2014; 11 (8): 506–14
- Patel, et al. Clin Perinatol. 2013;40(1):11-25.
- Shamir, et al. Gut Health in Early Life: Significance of the Gut Microbiota and Nutrition for Development and Future Health. 2015; John Wiley and Son.
- Vighi, et al. Clinical and Experimental Immunology.2008;153:3-6.
- Tibbs, et al. Microbial Cell. 2019;6(8): 324 – 334.
- Harm Wopersis, et al. Pediatr Allergy Immunol. 2014;25(5):428-38.
- Belkaid, et al. Cell. 2014;157(1):121-41.
- O'Hara, et al. EMBO Rep. 2006;7(7):688-93.
- McDermott, et al. Immunology. 2014;142(1):24-31.
- Belizário, et al. Exp Suppl. 2018;109:459-476.
- DeGruttola, et al. Inflamm Bowel Dis. 2016;22(5):1137-50.
- Carding, et al. Microb Ecol Health Dis. 2015;V26:26191
- Hawrelak, et at. Altern Med Rev. 2004;9(2):180-197
- Lee, et al. J Paediatr Child Health. 2017;53(12):1152-1158.
- Prescott, et al. J Allergy Clin Immunol. 2013;131(1):23-30
- Moossavi, et al. Front Pediatr. 2018 Jul 24;6:197.
- Jeurink, et al. Benef Microbes. 2013;4(1):17-30.
- Corona, et al. Children (Basel). 2021 Sep 14;8(9):804.
- Dong, et al. Saudi J Biol Sci. 2018;25(5):875-880.
- Candy, et al. Pediatr Res. 2018;83(3):677–86.
- Liu, et al. Front Nutr. 2022;8:634897.
- Sorensen, et al. Nutrients. 2021;13(7): 2205.
- NICE. Cow’s milk allergy in children. [online]. https://cks.nice.org.uk/topics/cows-milk-allergy-in-children/#:~:text=Cow%27s%20milk%20allergy%20is%20a,more%20proteins%20in%20cow%27s%20milk [accessed Feb 2026].
- Luyt, et al. Clin Exp Allergy. 2014;44(5):642-672.
- Allergy UK [online]. Does My Child Have a Cow's Milk Allergy? | Allergy UK | National Charity [accessed Feb 2026]
- Hubbard, et al. Immune inflamm & Dis. 2022;10(6):e636.
- Market comparison of UK EHF and AAF data cards, February, 2026.
- Abrahamse-Berkeveld, et al. J Nutr Sci. 2016;5:e42.
- Burks, et al. Pediatr Allergy Immunol.2015;26(4):316–22.
- Fox, et al. Clin Transl Allergy. 2019;9:5.
- van der Aa, et al. Clin Exp Allergy. 2010;40(5):795–804.
- Sorensen, et al. Nutrients. 2021;13(3):935.
- van der Aa, et al. Allergy. 2011;66(2):170-7.
- Martin, et al. Benef Microbes. 2010;1(4):367–82.
- Wopereis, et al. Pediatr Allergy Immunol. 2014;25(5):428–38.
- Harvey, et al. Pediatr Res. 2014;75(2):343–51.
- Walker, et al. Pediatr Res. 2015;77(1):220–8.
- West, et al. J Allergy Clin Immunol. 2015;135(1):3-13.
FOOTNOTES :
* SYNEO synbiotic blend: Bifidobacterium breve M-16V (probiotic) & short and long-chain galacto- and/or fructo-oligosaccharides (prebiotic). The only synbiotic blend within hypoallergenic formulas in the UK.30
†Aptamil Pepti Syneo and Neocate Syneo contain more of the gut microbiota modulating factors in breastmilk (prebiotic oligosaccharides [short and long-chain galacto- and/or fructo-oligosaccharides], probiotic bacteria [Bifidobacterium breve M-16V] and lactose [Aptamil Pepti Syneo only]) than any other hypoallergenic formulas in the UK.30
‡12 week RCT 34, Infants with Atopic Dermatitis, Aptamil Pepti Syneo vs non-synbiotic EHF; Systematic review and meta-analysis of 4 RCTs35, Neocate Syneo vs Neocate LCP (Nov 2020); Single arm UK non-IgE mediated CMA study29, baseline non-synbiotic formula (n=27 out of n=29 well established on a non-synbiotic EHF) vs Aptamil Pepti Syneo, 4 week intervention Follow-up arm of study n=13; 1 year follow up36 from 12 week RCT34; Observational study of real-world evidence in The Health Improvement Network (THIN) GP database25, n=148 Neocate Syneo vs Alfamino (Feb 2021).
Help us provide information most relevant to you
Please ensure your role and areas of interest are up to date.