Nutrison Diason Energy HP
A unique tube feed specifically designed for patients with hyperglycaemia

Inpatients are at risk of poor glycaemic control1,2.
Nutritional support strategies for patients with hyperglycaemia
Enteral tube feeds have been found to produce a more rapid rise in blood glucose levels than a nutritionally equivalent solid meal.

Controlling blood glucose levels may improve patient outcomes - patient safety and cost4,5
Causes of hyperglycaemia
The underlying cause of hyperglycaemia is usually loss of insulin producing cells in the pancreas or development of resistance to insulin
Contributing factors of hyperglycaemia
- Missing a dose of diabetic medication, tablets or insulin5
- New medication or change in medication, e.g. steroids5
- Overfeeding6
- Stress - physical (e.g. an injury or surgery), mental or emotional
- Infection of illness7
Symptoms of hyperglycaemia
Patient types at risk of hyperglycaemia
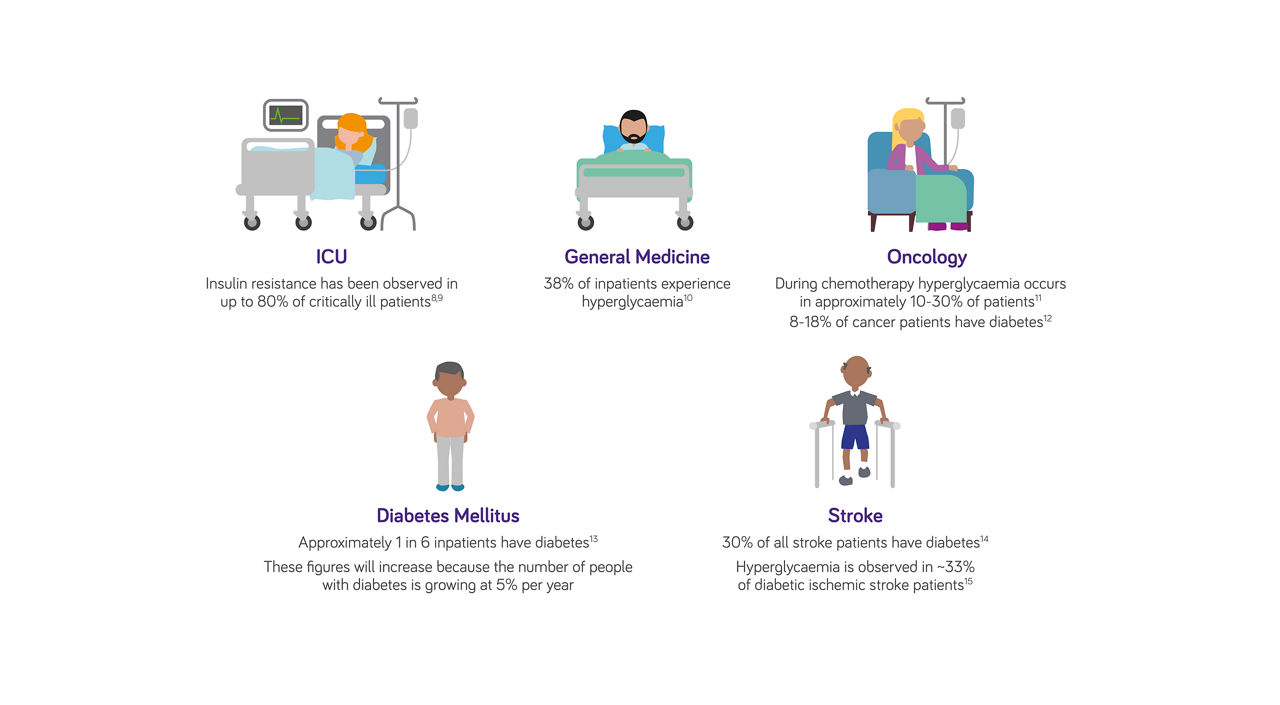
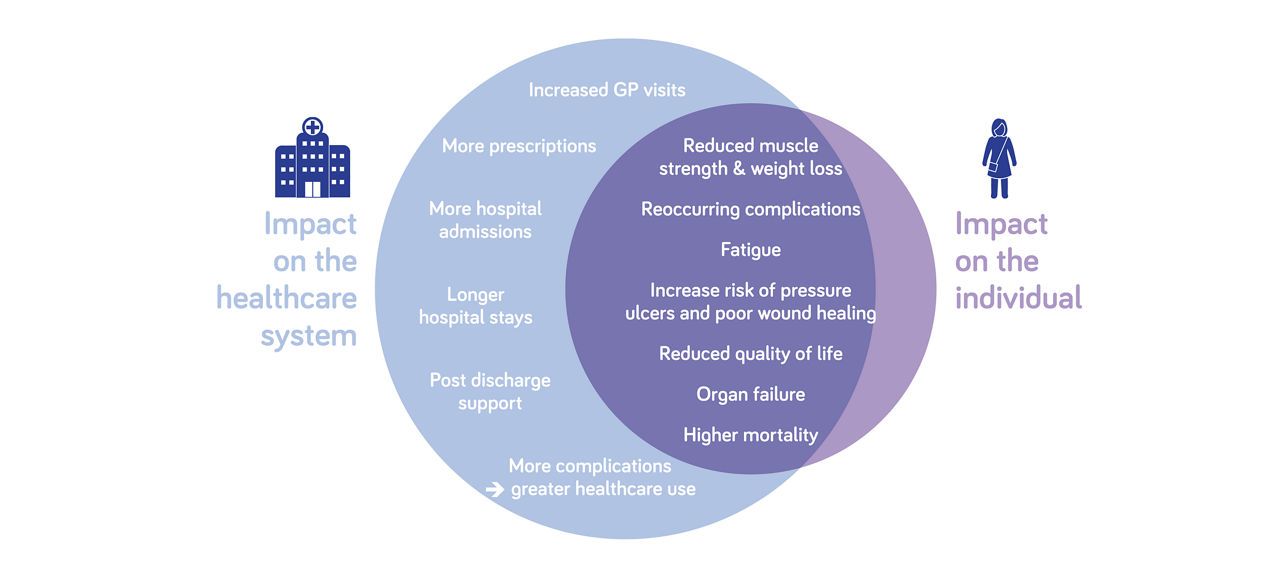
The impact of hyperglycaemia16-18
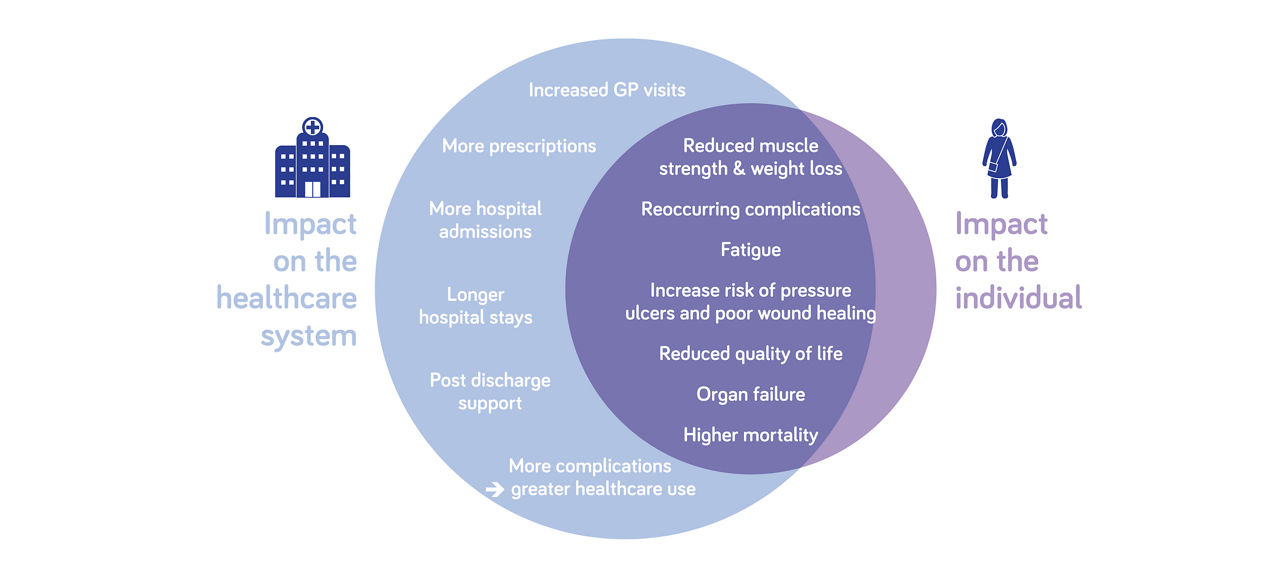
Managing tube fed patients with hyperglycaemia
Multidisciplinary team approach
Goals of dietetic intervention:
- Prioritise meeting the patient's nutritional requirements
- Monitor carbohydrate intake
- Communicate with the multidisciplary team
- Switch feeding method - bolus vs continuous
- Trying a slower feeding rate
- Try a high protein or high fibre tube feed
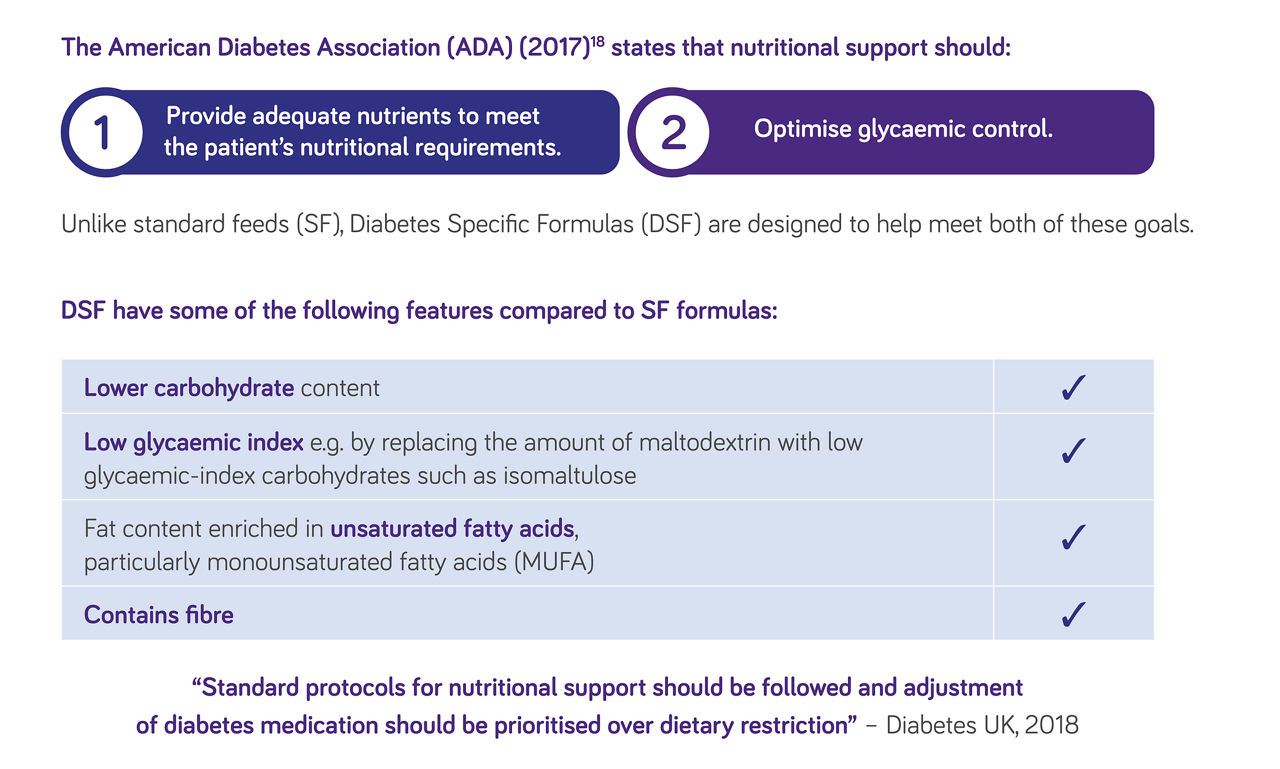
What are diabetes specific formulas?16-18
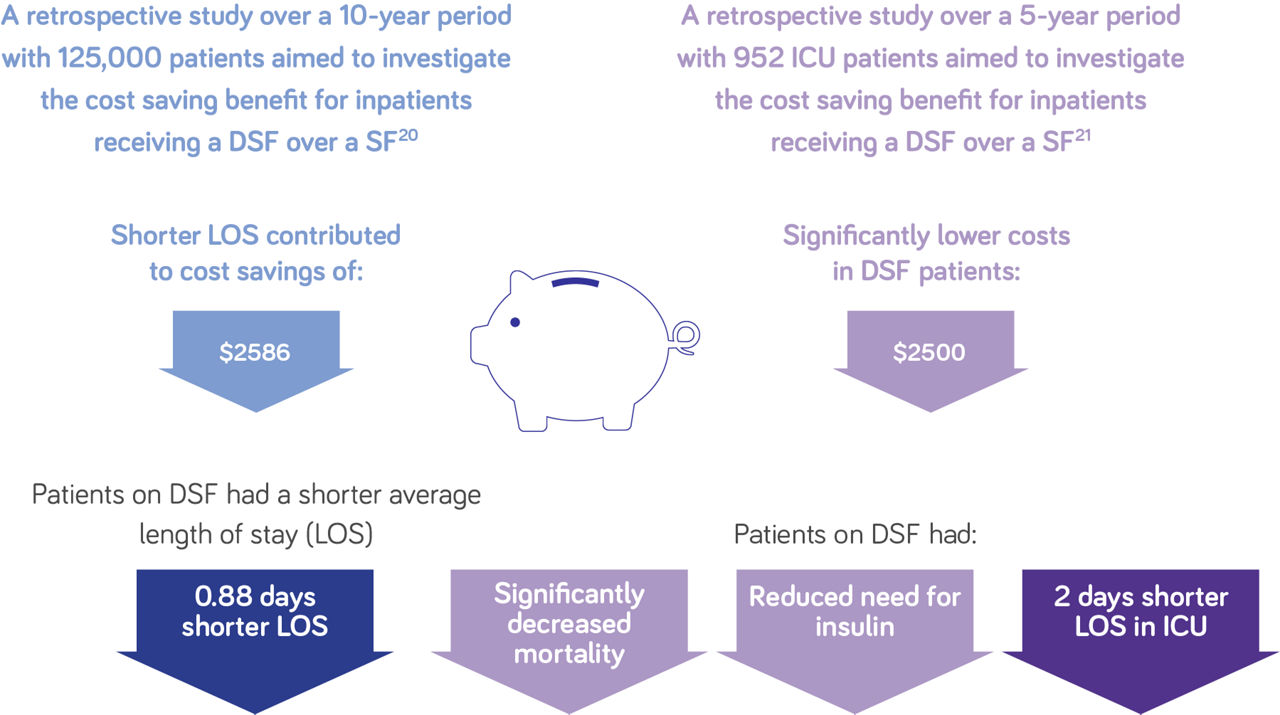
Clinical benefits of diabetes specific formulas

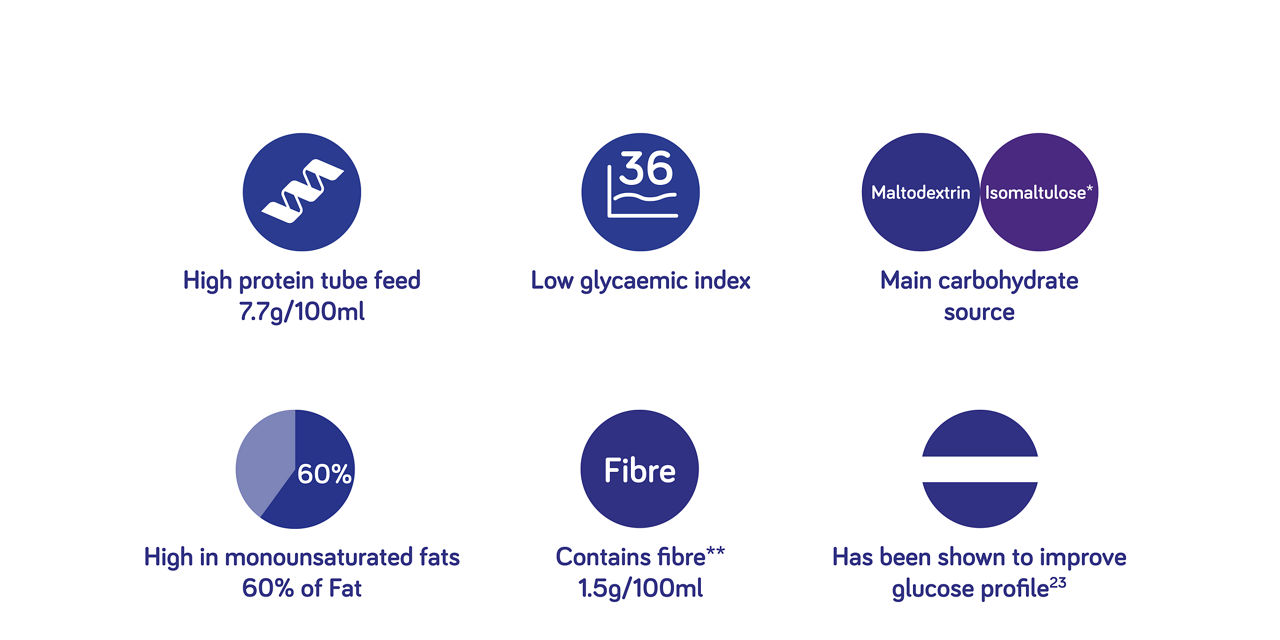
A UNIQUE tube feed designed for patients with hyperglycaemia
*Isomaltulose has a slow hydrolysis rate resulting in a reduced glucose and insulin response24
**A mixture of soluble and insoluble fibres to help maintain gut health including gut integrity and bowel function25
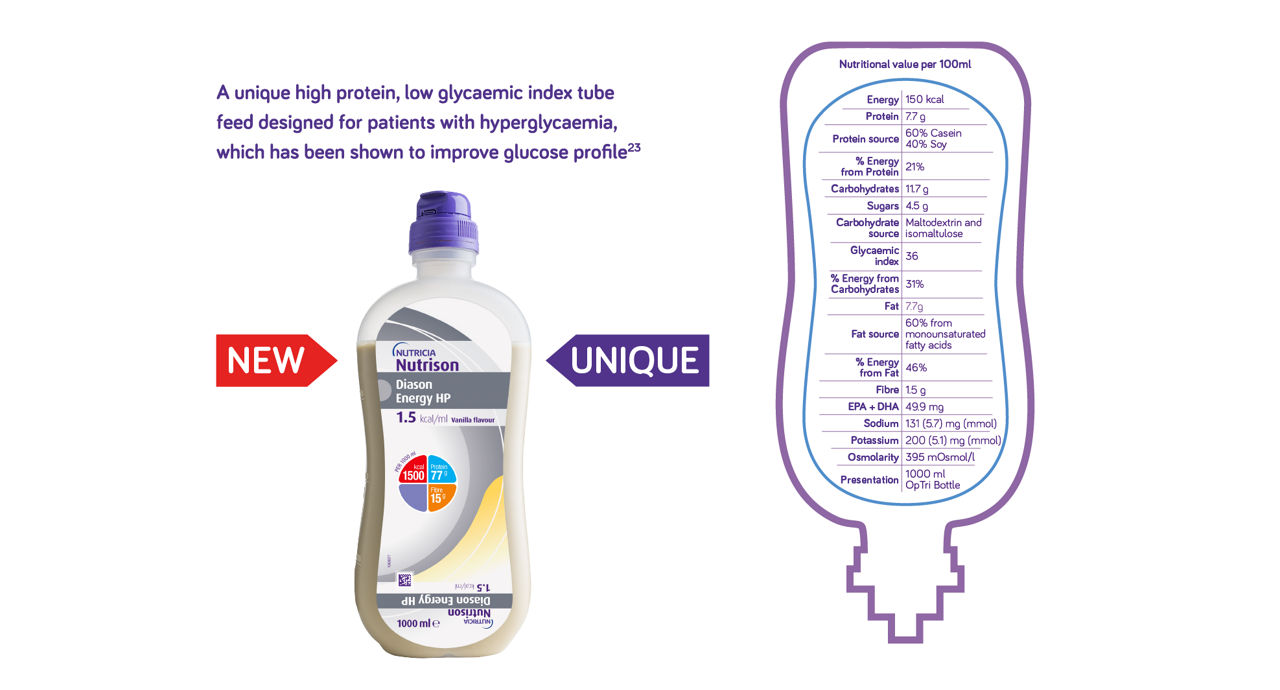
Nutrison Diason Energy HP has been proven to improve glucose levels23
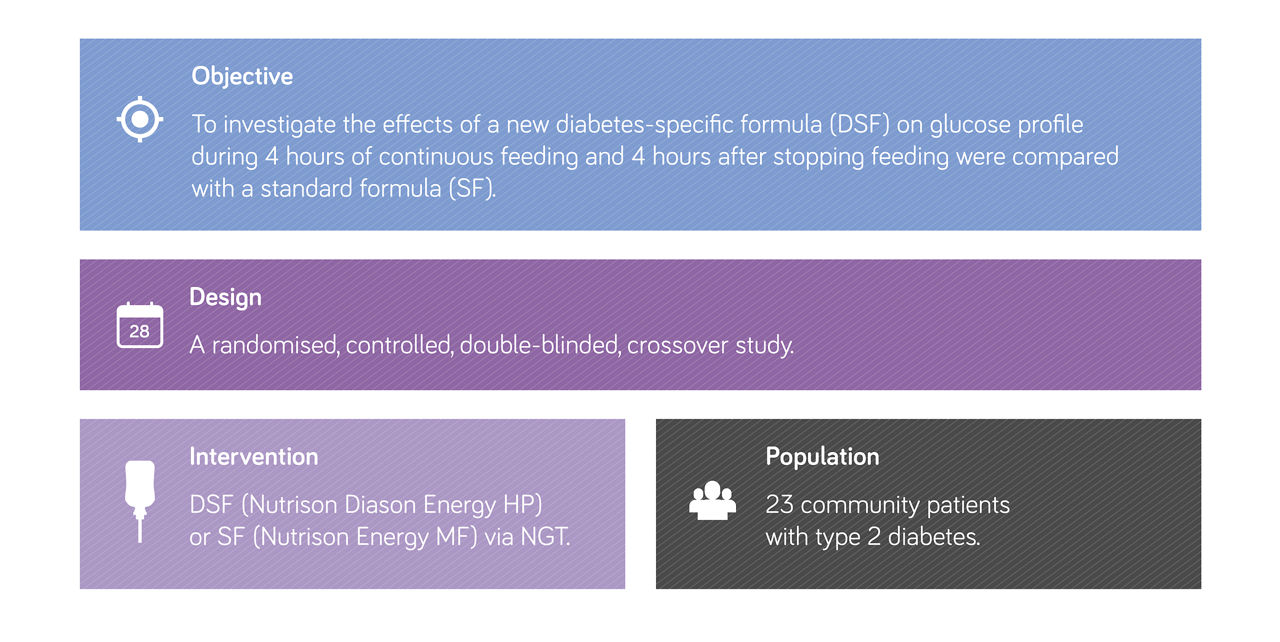
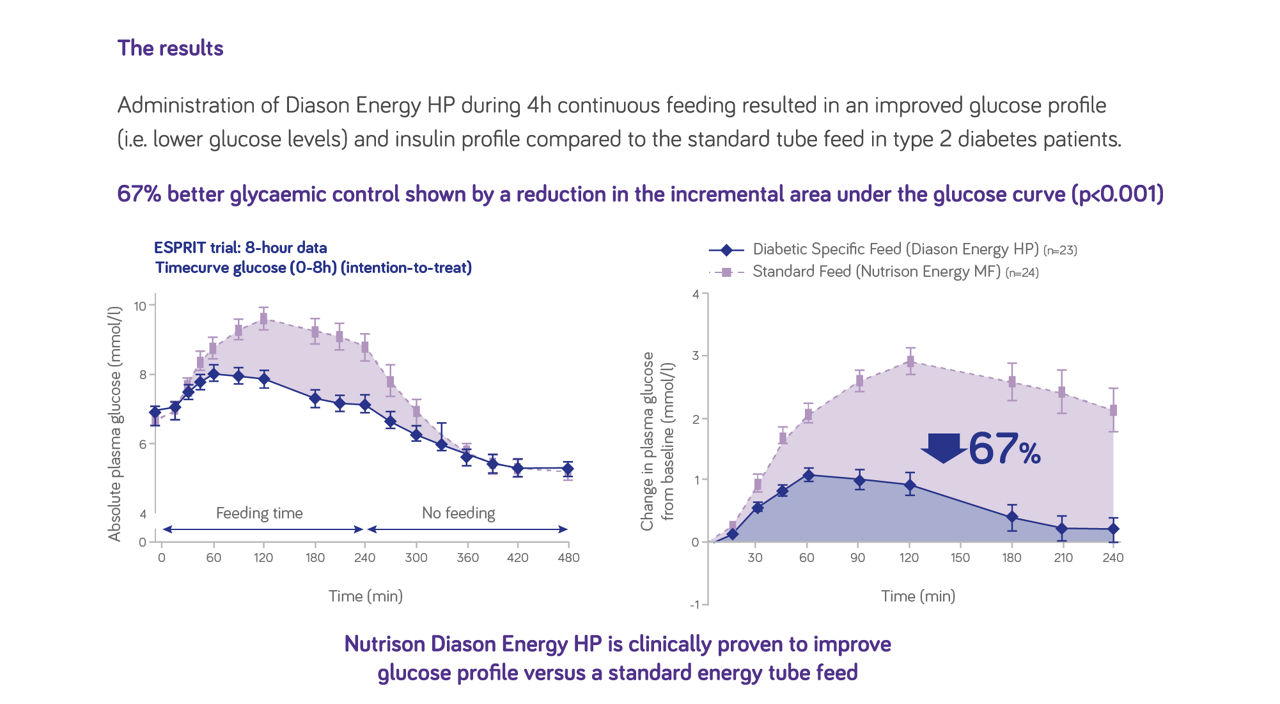
- World Health Organization, 2006. Definition and diagnosis of diabetes mellitus and intermediate hyperglycaemia.
- Gandy J. 2015. Manual of Dietetic Practice.
- Pancorbo-Hidalgo PL, et al. Complications associated with enteral nutrition by nasogastric tube in an internal medicine unit. J Clin Nurs. 2001; 10(4):482-90.
- McMahon MM, et al. A.S.P.E.N. clinical guidelines: nutrition support of adult patients with hyperglycemia. JPEN J Parenter Enteral Nutr. 2013; 37(1):23-36. https://aspenjournals.onlinelibrary.wiley.com/doi epdf/10.1177/0148607112452001
- Davidson P, et al. Management of Hyperglycemia and Enteral Nutrition in the Hospitalized Patient. Nutr Clin Pract. 2015; 30(5):652-9.
- González Infantino CA, et al. Hyperglycemia and hypoalbuminemia as prognostic mortality factors in patients with enteral feeding. Nutrition. 2013; 29(3):497-501.
- Meizoso JP, et al. Admission hyperglycemia is associated with different outcomes after blunt versus penetrating trauma. J Surg Res. 2016; 206(1):83-9.
- Honiden S, et al. Metabolic Management during Critical Illness: Glycemic Control in the ICU. Semin Respir Crit Care Med. 2015; 36(6):859-69. https://www.thieme-connect.com/products/ejournals/pdf/10.1055/s-0035-1565253.pdf
- Plummer MP, et al. Dysglycaemia in the critically ill and the interaction of chronic and acute glycaemia with mortality. Intensive Care Med. 2014; 40(7):973-80.
- Umpierrez GE, et al. Hyperglycemia: an independent marker of in-hospital mortality in patients with undiagnosed diabetes. J Clin Endocrinol Metab. 2002; 87(3):978-82. https://academic.oup.com/jcem/article/87/3/978/2846522
- Hwangbo Y, et al. Acute Hyperglycemia Associated with Anti-Cancer Medication. Endocrinol Metab (Seoul). 2017; 32(1):23-9. https://www.e-enm.org/upload/pdf/enm-32-23.pdf
- Habib SL, et al. Diabetes and risk of cancer. ISRN Oncology. 2013; 2013:583786.
- National Diabetes Audit, 2017.
- Lau LH, et al. Prevalence of diabetes and its effects on stroke outcomes: A meta-analysis and literature review. J Diabetes Investig. 2019; 10(3):780-92. https://onlinelibrary.wiley.com/doi/epdf/10.1111/jdi.12932
- Mi D, et al. Correlation of hyperglycemia with mortality after acute ischemic stroke. Ther Adv Neurol Disord. 2017; 11:1756285617731686. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5784549/
- Elia M, et al. Enteral nutritional support and use of diabetes-specific formulas for patients with diabetes: a systematic review and meta-analysis. Diabetes Care. 2005; 28(9):2267-79. https://care.diabetesjournals.org/content/28/9/2267.long
- Ojo O, et al. Evaluation of the role of enteral nutrition in managing patients with diabetes: a systematic review. Nutrients. 2014; 6(11):5142-52. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4245584/
- American Diabetes Association. Diabetes Care in the Hospital. Diabetes Care. 2017; 40(Suppl 1).
- Sanz-París A, et al. Diabetes-specific formulas high in monounsaturated fatty acids and metabolic outcomes in patients with diabetes or hyperglycaemia. A systematic review and meta-analysis. Clin Nutr. 2020; 39(11):3273-82.
- Hamdy O, et al. Differences in resource utilization between patients with diabetes receiving glycemia-targeted specialized nutrition vs standard nutrition formulas in U.S. hospitals. JPEN J Parenter Enteral Nutr. 2014; 38(2 Suppl):86s-91s.
- Han YY, et al. The clinical and economic impact of the use of diabetes-specific enteral formula on ICU patients with type 2 diabetes. Clin Nutr. 2017; 36(6):1567-72.
- Barazzoni R, et al. Carbohydrates and insulin resistance in clinical nutrition: Recommendations from the ESPEN expert group. Clin Nutr. 2017; 36(2):355-63.
- Lansink M, et al. Improved Glucose Profile in Patients With Type 2 Diabetes With a New, High-Protein, Diabetes-Specific Tube Feed During 4 Hours of Continuous Feeding. JPEN J Parenter Enteral Nutr. 2017; 41(6):968-75.
- Lina BAR, et al. Isomaltulose (Palatinose®): a review of biological and toxicological studies. Food and Chemical Toxicology. 2002; 40(10):1375-81.
- Green CJ. Fibre in enteral nutrition. Clinical Nutrition. 2001; 20(1):23-39.
Help us provide information most relevant to you
Please ensure your role and areas of interest are up to date.



