Prebiotic oligosaccharides: supporting gut health in preterm infants – a guide for healthcare professionals
In this guide for healthcare professionals, we take a look at the importance of supporting the gut microbiota and the role that prebiotics can play in creating positive health outcomes in preterm infants.

Every year 15 million infants around the world are born too early and before completion of the 37th week of pregnancy, and preterm birth is the number one cause of child mortality around the world1.
Infants who are born prematurely often face multiple health concerns, including feed intolerance, poor gut barrier function and increased risk of infection2-4. The gut microbiota in these infants is considered to be important for protection against harmful microorganisms and for the maturation of the immune system5. Increasing evidence suggests that promoting a healthy microbiota is key to supporting the best possible outcomes in preterm infants3.
Good nutritional support of preterm infants has been shown to improve neonatal growth and developmental outcomes, including brain development, to support optimal long term health6,7.
The benefits of breast milk on the microbiota
Breast milk is universally recognised as promoting the best health outcomes in both preterm and term infants by providing a unique combination of nutrients and immune-protective factors8,9. A key benefit of breast milk is the promotion of a healthy gut microbiota, which is in part attributed to the presence of prebiotic oligosaccharides (OS) supporting gut intestinal flora development (figure 1)4,10.
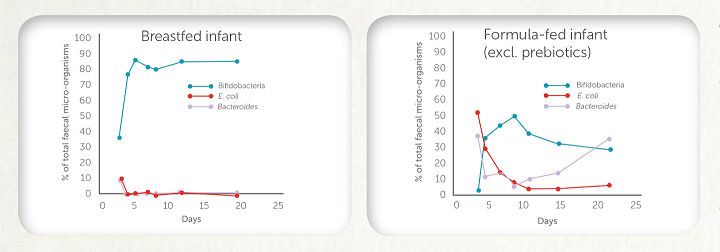
Figure 1
Adapted from: Harmsen, et al. 2000 Figure 1 – The microbiota of breastfed newborn infants is dominated by beneficial bifidobacteria (up to 90%) and has lower levels of harmful bacteria (such as E. coli and Bacteroides) compared to infants fed a formula without prebiotics during the first 20 days of life10.
Prebiotic oligosaccharides positively influence the gut microbiota
If breast milk is not available or available in sufficient amounts for a preterm infant, a specific preterm formula is recommended11. Several clinical studies have proven that a formula containing prebiotic OS (compared to a formula without prebiotic OS) helps to support the preterm gut microbiota in a number of different ways:
- Increasing the number of bifidobacteria in the gut (Figure 2)12.
- Promoting stool frequency patterns and consistency similar to breast milk fed infants12,13.
- Reducing numbers of potentially pathogenic bacteria in the gut14.
- Potentially improving enteral tolerance in very preterm infants13,15.
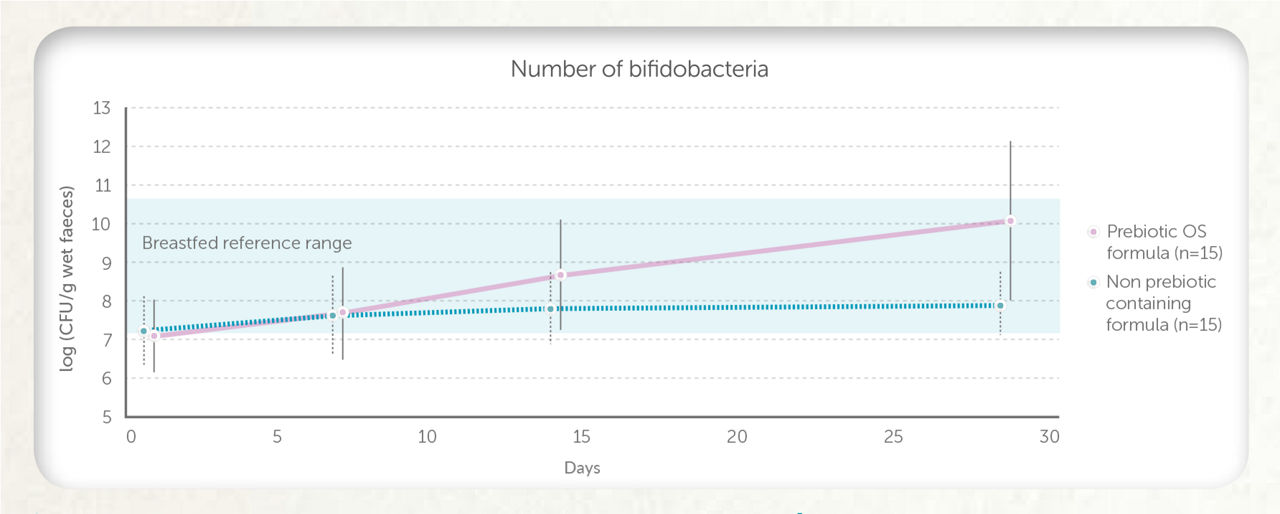
Figure 2
Adapted from: Boehm, et al. 2002 Figure 2 – Preterm infants receiving a preterm formula with prebiotic OS for 28 days had significantly higher levels of bifidobacteria in the gut, compared to the group receiving a formula without prebiotic OS (p=0.0008).12
40 years of early life science
At Nutricia we have over 40 years of breast milk expertise with a dedicated team of around 250 specialist scientists collaborating with hospitals, laboratories and universities worldwide to ensure we’re leaders in this field. Science is at the heart of our nutrition and health commitment to help healthcare professionals support parents during the first 1,000 days. Our research and innovation delivers evidence-based nutritional solutions to support a child’s lifelong health, combining our Early Life Nutrition expertise with years of professional experience to develop a portfolio of products to support the nutritional needs of mums, mums-to-be, parents and partners and their babies.

